Addressing Healthcare Inequity Through Empathy & Innovation
A Design Thinking Approach to Revolutionizing Healthcare Access
Estimated Read Time: 3 Minutes
The COVID-19 pandemic has exposed a dramatic, yet often overlooked, issue within the US healthcare system – disparities in care and outcomes based on social, racial, ethnic, economic, and environmental factors. These disparities are deeply rooted in the “social determinants of health,” which play a critical role in influencing an individual’s well-being and health. These determinants include factors such as socioeconomic conditions, physical environment, and health behaviors, which are complex social issues that require long-term solutions and involve more than just healthcare providers.
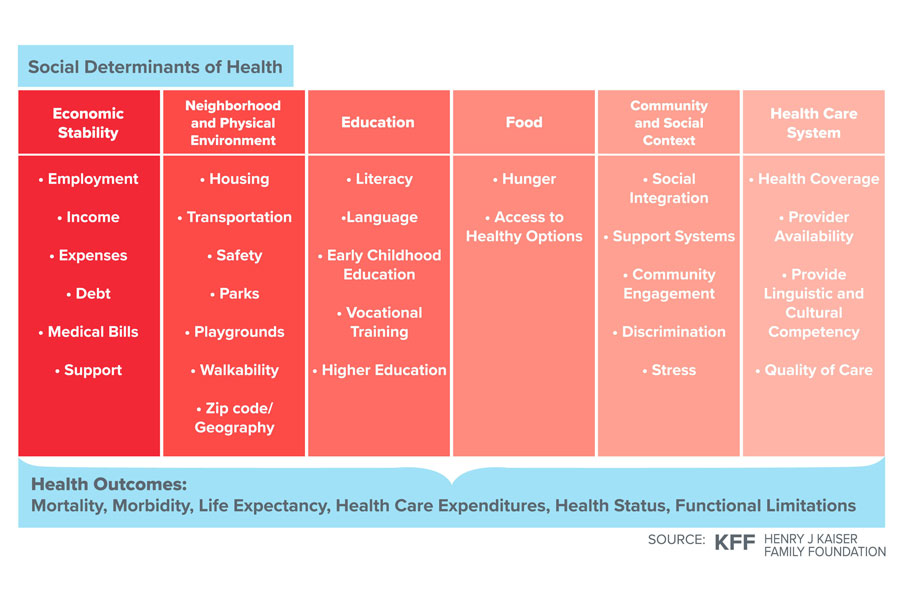

While 80% of a person’s health is impacted by these social determinants of health, there is a crucial 20% of health outcomes related to access and healthcare equality that can and should be addressed immediately.
Access to healthcare manifests in many dimensions, including physical access, but also access to online tools, transportation and mobility, financial support, and language accessibility. Limits to physical access has been especially exacerbated as many healthcare organizations move out of poorer neighborhoods and build facilities in more affluent areas to capture market share. While such a decision might be financially sound, it raises questions about the mission and values of healthcare providers. Creativity, empathy, and innovative thinking are required to bridge this gap effectively. Mere physical presence is insufficient; the ability to relate to patients, communicate effectively, understand their struggles, and provide respectful and dignified care is equally crucial.
Providing sufficient access also involves creatively addressing issues related to:
- Transportation
- Language
- Human empathy
- Creative financing
- Community reach

Health systems across the country have shown increasing interest in addressing these inequities we all see. Nevertheless, it can be a daunting task. In our field, we are accustomed to tackling complex problems. A handy tool is the application of a process known as design thinking. By applying design thinking principles and processes, teams can collectively and collaboratively make significant progress toward meaningful solutions. Here are some starting points:
- Empathy: Design thinking begins with the collection and absorption of insights into the consumer (patient) and their needs. We often utilize in-depth qualitative techniques to probe how consumers think, feel and behave related to the issues at hand. These techniques include shadowing, in-home ethnography, diaries, and projective exercises. Using these tools, we can dive into consumers’ thoughts, feelings, and behaviors related to the issue at hand. This enables profound understanding of the problems, barriers, aspirations, and ideals of the individuals.
- Experience Mapping: Armed with empathetic insights, it is valuable to map the consumer’s/patient’s experience across stages of their health journey, addressing not only the treatment but the holistic experience. Identifying specific pain points and pivotal moments across these stages provides opportunities for breakthrough thinking and concepts. This mapping typically covers both the current state and the ideal state from the customer’s perspective.
- Definition: Documentation of the insights and experience mapping are consolidated into a series of experience principles and themes that define the problems to be addressed and the desired end-state outcomes from the customer’s perspective.
- Ideation: A well-defined problem statement and identified opportunities serve as a foundation for generating creative solutions. These solutions should be centered around the consumer/patient, considering how care teams and operations can enable them. Emulators and experiences from other industries can stimulate innovative thinking. The process involves cross-functional teams that brainstorm ideas, prioritize them, and visualize concepts.
- Prototyping: Prioritized ideas are translated into various mock-ups, ranging from low fidelity to higher fidelity versions of solutions. This may involve concept narratives, 3D renderings and virtual fly-throughs, digital or interactive tool prototypes, and more, providing visual and tangible representation of the proposed solution.
- Test and Learn: Armed with prototypes or mock-ups, consumers/patients are presented with the ideas and concepts to gain feedback and insights. This iterative process aims to refine and improve ideas before implementing them in a pilot phase.
Learn more about test and learn approach »
Healthcare organizations, by their very mission and mandate, serve diverse populations. However, this doesn’t imply that a one-size-fits-all approach is suitable. Different communities and populations have different needs, challenges, aspirations, and desires. It is often hard to apply one’s own lived situation and generate solutions for someone with radically different life realities. To address inequities and disparities in healthcare access, a deeply empathetic and innovative approach is essential to create experiences tailored specifically for these communities, not just meeting their needs but also delighting and engaging them.
While the process mentioned can certainly be managed by internal teams, WD Partners is prepared to serve as an innovation partner, offering guidance and creative thinking to complement your healthcare teams in this crucial journey.